Early diagnosis of Primary Ciliary Dyskinesia (PCD) remains one of...
Read MorePorts and Tune Ups in PCD: What Families Need to Know
For many people living with Primary Ciliary Dyskinesia (PCD), treatment is not only about managing acute infections. It is also about reducing the long-term cycle of mucus retention, inflammation, and progressive lung damage that can occur when the airways cannot clear properly. In PCD, impaired mucociliary clearance leads to a build-up of secretions in the lungs, which can contribute to chronic infection and inflammation over time.
One treatment families may hear about is a “tune up.” This is an informal term often used to describe a planned course of intravenous (IV) antibiotics, commonly given over around two weeks. A tune up is not always used to treat a sudden acute infection. In some children and adults with chronic suppurative lung disease, including PCD, IV antibiotics may also be used at intervals to reduce bacterial load, calm inflammation, and help bring symptoms and lung health back under better control.
What is a port?
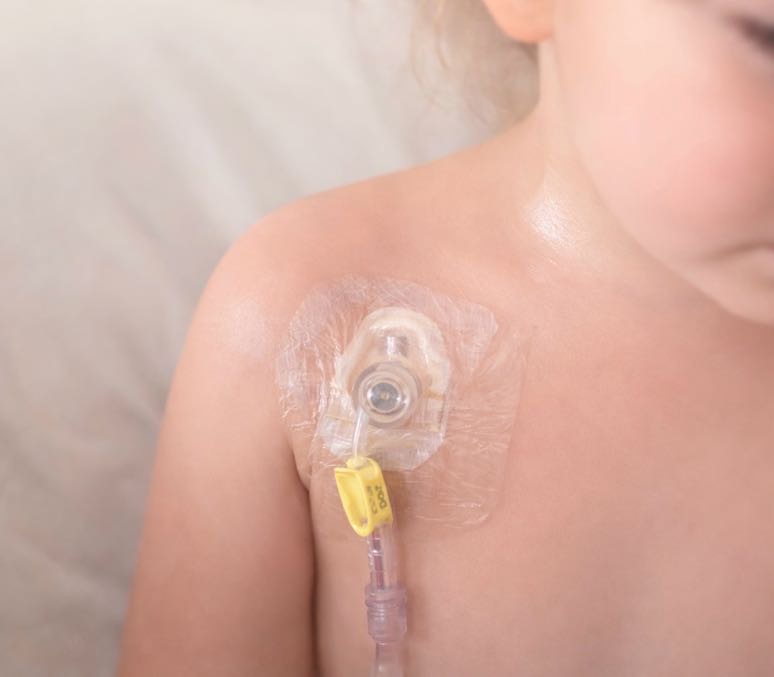
A port, also called an implantable venous access device (IVAD), is a type of central venous access device placed completely under the skin. It has a small chamber under the skin connected to a catheter, with the catheter tip sitting in a large vein close to the heart. Medicines, fluids and blood tests can be given or taken through the port when it is accessed with a special needle.
Ports are designed for adults and children who need more reliable long-term IV access. Unlike a standard cannula, which is short-term, a port can remain in place for months or years if it is functioning well and still needed for treatment.
Why might a child with PCD need one?
For some children with PCD, repeated IV treatment becomes a regular part of life. Over time, repeated cannulas or other temporary lines can become distressing, difficult to place, or simply impractical. A port may be recommended when a child needs frequent or ongoing IV medications, has small or difficult veins, or requires longer-term treatment access. It can also make blood collection easier, reducing the need for repeated needle insertions elsewhere.
A port is not the default option for every child with PCD. The choice depends on how often IV treatment is needed, how difficult IV access has become, what other lines have been used before, and the child’s overall treatment plan.
Claudette’s story
Claudette is a three-year-old child in Sydney living with PCD. In March 2026, she received a port so she could have two weeks of IV antibiotics every three months as part of her treatment plan.
For children like Claudette, a port is usually not a first step. It is often considered after other access options have been used repeatedly and are no longer the most practical or effective way to deliver regular treatment. In that setting, a port can become an important tool in ongoing care.
What families can expect
A port is inserted during a surgical procedure under general anaesthetic. Because the port sits fully under the skin, there is no external line when it is not being used. Children are usually sore around the incision sites for a few days afterwards, and the treating team will explain how to care for the area while it heals. Sydney Children’s Hospitals notes that soreness around the insertion sites is common for about a week after insertion.
Living with a port
One of the benefits of a port is that when it is not accessed, it is mostly hidden under the skin and many children can return to normal day-to-day activities once the site has healed. Children can usually go back to daycare or school, and many normal activities can continue. Guidance from children’s hospitals notes that swimming is generally possible when the port is not accessed, but when the port is accessed with a needle and dressing in place, it should not be submerged in water. Families should also ask their treating team for advice about contact sports or rough play.
Ports do still require ongoing maintenance. When not in regular use, they need to be flushed and locked regularly by a port-trained healthcare professional to help reduce the risk of blockage and infection. Ports can last a long time, but in children they may eventually need to be replaced as the child grows, if the device is no longer positioned correctly, or if complications occur.
When should families seek help?
Families are taught what warning signs to watch for. These can include fever, redness, swelling, heat, pain, discharge, or problems using the port. Sydney Children’s Hospitals advises that if a child with a port has a temperature of 38°C or higher, they should present for urgent medical review because the port can be a possible source of infection.
A treatment tool, not a setback
For families new to the idea, hearing that a child needs a port can feel overwhelming. But in many cases, it represents a move toward more sustainable, planned care. It can reduce trauma from repeated needle attempts, make regular treatment more achievable, and support children who need ongoing IV antibiotics as part of managing their lung disease.
In PCD, where treatment is often long-term and cumulative, a port can become one more practical tool in protecting lung health over time.
Recent Posts
Lung Legends
We are proud to share that Lung Foundation Australia has...
Read MorePCD and Fertility: Can People with Primary Ciliary Dyskinesia Have Children?
Primary Ciliary Dyskinesia (PCD) is a rare genetic condition that...
Read MorePorts and Tune Ups in PCD: What Families Need to Know
For many people living with Primary Ciliary Dyskinesia (PCD), treatment...
Read More