We are proud to share that Lung Foundation Australia has...
Read MoreThe Path to PCD Diagnosis: Understanding PICADAR and Early Detection
Early diagnosis of Primary Ciliary Dyskinesia (PCD) remains one of the biggest challenges for families and clinicians. Because PCD is a rare genetic condition with symptoms that overlap with many other respiratory illnesses, children can often go years without an accurate diagnosis.
In Australia, where access to specialised diagnostics can be limited, it is possible that someone with PCD may develop bronchiectasis and be treated for bronchiectasis without ever identifying PCD as the underlying cause.
To help clinicians identify patients who may need further testing for PCD, researchers developed a clinical prediction tool called PICADAR.
You can read the original research here:
https://pmc.ncbi.nlm.nih.gov/articles/PMC4819882/
PICADAR is a simple scoring system based on seven clinical features commonly seen in people with PCD. By evaluating these factors, clinicians can estimate the likelihood that a patient’s symptoms may be caused by PCD and determine whether specialised diagnostic testing should be considered.
The tool was first developed and validated in respiratory clinics and has since become widely used internationally to help guide referrals for PCD diagnostic assessment.
The 7 Predictive Parameters of PICADAR
The PICADAR score evaluates seven clinical features in patients with persistent respiratory symptoms:
1. Full-Term Birth
Many children with PCD are born at full term rather than prematurely. This detail can help differentiate PCD from conditions more commonly associated with prematurity.
2. Neonatal Chest Symptoms
Respiratory distress in the first days of life is a common early sign of PCD. Newborns may require oxygen support or show breathing difficulties shortly after birth.
3. Admission to a Neonatal Unit
Because of early breathing problems, babies with PCD are more likely to be admitted to a neonatal intensive care or special care nursery shortly after birth.
4. Chronic Rhinitis
Children with PCD often experience persistent nasal congestion and a runny nose from a very young age. This chronic rhinitis typically continues throughout childhood.
5. Ear Symptoms or Hearing Problems
Recurrent ear infections and hearing difficulties are frequently seen in children with PCD due to impaired mucus clearance in the middle ear.
6. Situs Inversus
Around half of people with PCD have a condition called situs inversus, where internal organs are mirrored from their normal positions. When this is present alongside chronic respiratory symptoms, it can be a strong clinical indicator.
7. Congenital Heart Defects
Some individuals with PCD also have congenital heart abnormalities, which can occur alongside the underlying developmental differences affecting the body’s cilia.
These seven factors are combined into a score that helps clinicians estimate the probability of a PCD diagnosis.
How the PICADAR Score Works
Each of these features contributes to an overall score, which estimates the probability of a PCD diagnosis.
A higher score indicates a greater likelihood of PCD, helping clinicians decide when to refer for specialised testing.
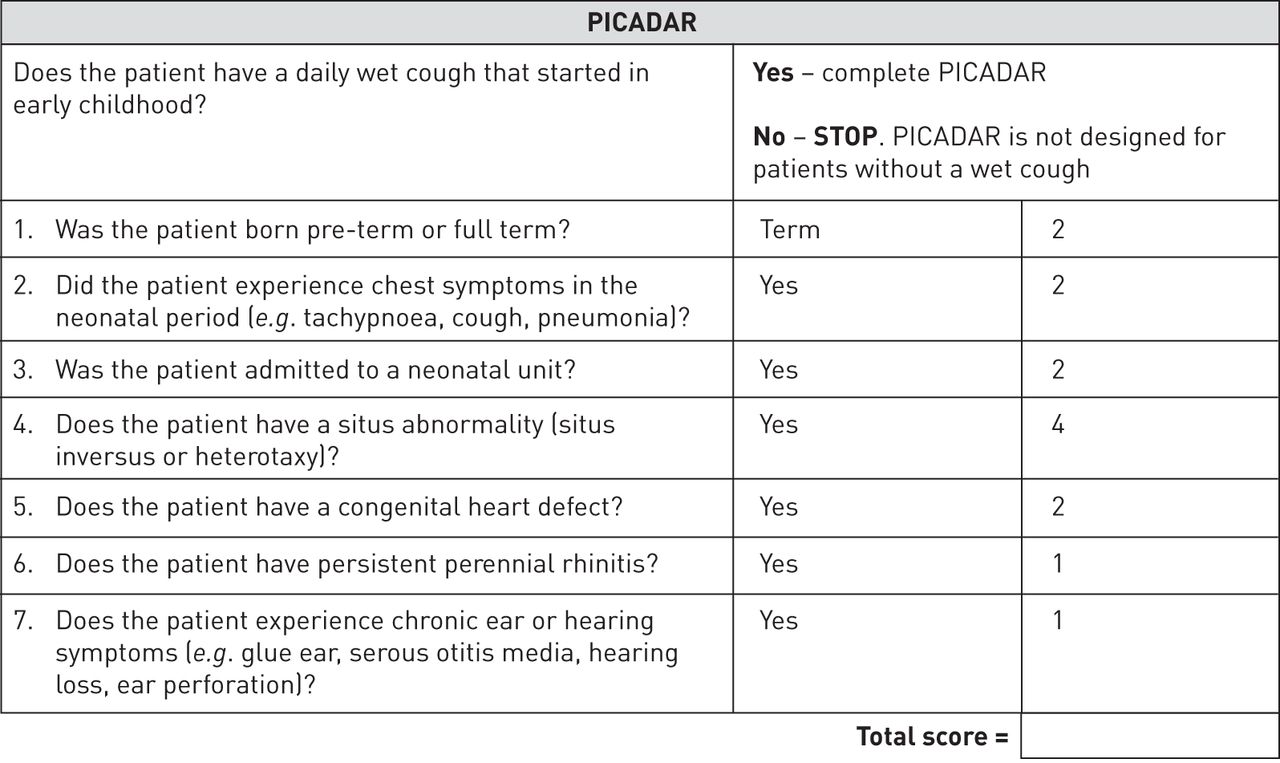
A maximum score of 14 points corresponds to a 99.8% probability of having PCD.
PICADAR Score and Probability of PCD
- Score 0–2: <1% probability
- Score 3: ~2% probability
- Score 4: ~5% probability
- Score 5: ~11% probability
- Score 6: ~24% probability
- Score 7: ~45% probability
- Score 8: ~68% probability
- Score 9: ~84% probability
- Score 10: ~93% probability
- Score 11: ~97% probability
- Score 12: ~98% probability
- Score 13: ~99% probability
- Score 14: ~99.8% probability
In clinical practice, a score of 5 or above is often used as a threshold to consider referral for further diagnostic testing.
Why Tools Like PICADAR Matter
For rare diseases like PCD, diagnostic delays are common. Many children experience years of recurring chest infections, chronic cough, or sinus disease before receiving the correct diagnosis.
Tools like PICADAR help clinicians recognise patterns earlier and ensure patients are referred to specialist diagnostic centres, where tests such as:
- Nasal nitric oxide measurement
- Genetic testing
- Ciliary function analysis
can be performed.
Earlier diagnosis allows families and healthcare teams to begin appropriate respiratory management sooner, helping to protect lung function and improve long-term outcomes.
Supporting Earlier Diagnosis in Australia
At PCD Australia, improving early recognition and diagnosis is one of our key priorities.
By raising awareness of clinical tools like PICADAR and advocating for improved diagnostic pathways, we aim to ensure Australians living with PCD receive timely access to specialist care.
Earlier diagnosis leads to better management, better support for families, and ultimately better outcomes for people living with PCD.
Recent Posts
You Don’t Know What You Know Until You Ask … So We Did
PCD Australia recently circulated a Listening Survey to gain a...
Read MoreThe Path to PCD Diagnosis: Understanding PICADAR and Early Detection
Early diagnosis of Primary Ciliary Dyskinesia (PCD) remains one of...
Read MorePorts and Tune Ups in PCD: What Families Need to Know
For many people living with Primary Ciliary Dyskinesia (PCD), treatment...
Read More